Obesity in Canada: No Quick Fix for a Complex Problem
Rising population-level obesity is a long-observed phenomenon in OECD countries. Canada is no exception to this rule. A recent report projects that, by 2025, 34% of Canadians will be obese. All levels of government have experimented with different policy solutions, and yet obesity continues to rise.
Recently, I was asked to write a brief analyzing Canada’s rising rate of obesity and recommend one federal policy that would mitigate the crisis. Ironically, there is no single solution to this complex issue. States around the globe have tried the quick-fix approach, crafting policies around single facets of the problem. With obesity, this typically means addressing either nutrition or physical activity rates. In terms of causality, obesity is linked to genetics, nutrition, and exercise. Government responses, to date, have not considered all three aspects. I’ve included some population data, below, which demonstrates that obesity cannot be solved with a single policy program.
Who is Obese in Canada?
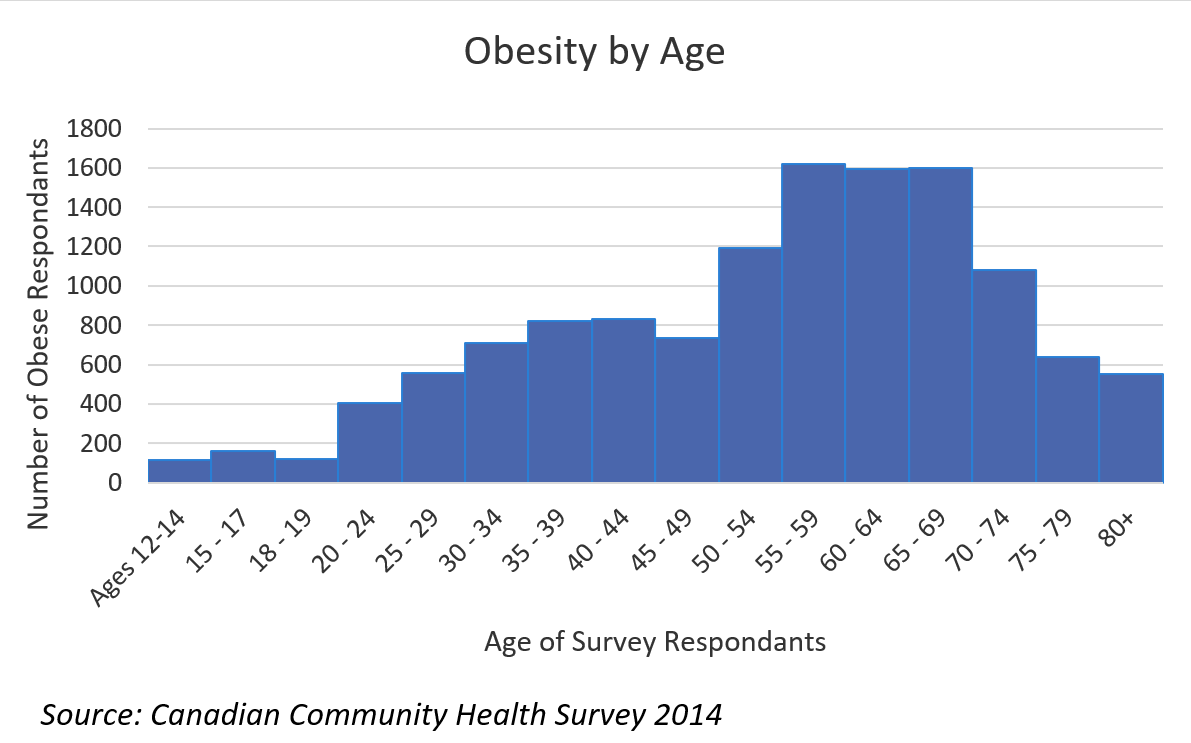
Getting a population-level understanding of who is at a healthy weight means using survey data generated by self-reports of height and weight. From there, Statistics Canada calculates respondents’ body mass index: a crude but cost-effective measure for obesity. The Canadian Community Health Survey (CCHS) is a widely cited dataset for understanding who is obese in Canada. In 2014, the most recent study period available for public use, of those individuals self-reporting obese-level heights and weights, 52% were female, and 48% were male. Examining the population above 12 years old, the distribution of obese individuals is right-skewed towards older individuals, centred around respondents between 50 and 74 years old.
Across income groups (no income and income quartiles), most survey respondents self-reporting obesity are from the low-income or no-income categories. When the income variable is applied across individual province populations, there is some variation. In Alberta and BC, obesity is higher among high-earning individuals (a right skewed distribution), while in the rest of Canada, obesity is skewed towards those with little to no income.
What Contributes to Obesity?
As mentioned earlier, obesity is largely the product of three factors: genetics, diet, and exercise. For the purposes of this article, however, I’m setting genetics aside. Not only are there ethical implications in genetics-based policy, but their role in determining obesity is contested. Diet, on the other hand, is generally considered a determining factor. Getting a balanced diet that includes fruits and vegetables is not as easy as it seems. Fast-food and other unhealthy options remain cheap, while healthier options are more expensive. In 2014, daily consumption of fruits and vegetables increased along income deciles. The more affluent a person is, the more fruits and vegetables they can afford.
Canada does not have a good track record when it comes to disseminating nutrition information. Medical experts have frequently critiqued the Canada Food Guide. Consequently, there is no real consensus on what constitutes ‘healthy’ versus ‘unhealthy’ food. In an era where ‘Fake News’ and Gwyneth Paltrow-like entrepreneurs prey on public ignorance, Canadians are poorly positioned to make the dietary choices which prevent obesity.
Policymakers should also consider barriers to physical exercise in their analysis. As previously demonstrated, those with lower incomes tend to have the highest risk of obesity. The 2014 CCHS shows that rigorous physical activity increases as wages increases. Canada is not unique in this trend. American data shows that high income earners are 31% more likely to exercise than those earning below $20,000 USD per year. Policies aimed at preventing obesity through exercise participation need to be cognizant of the labour-leisure constraints of these high-risk demographics.
Policy Choice 1: Nutrition
If the government chooses to target diet, there are two options. It can go after the unhealthy food supply or try to remove the cost barriers to healthy food. Taxing unhealthy foods is not a new policy idea. In 2012, France introduced a tax on drinks containing unhealthy levels of sugar or sweetener chemicals. This successfully decreased the sales of unhealthy beverages, but there was a minimal shift in population-level obesity. In the UK, debates over a proposed tax on red meat have raised the question of whether the government ought to tell people what to eat.
Subsidies are another instrument for behavioural change. Subsidies on healthy food options have been implemented around the world. A systematic review of 24 healthy food subsidy programs shows that, given a subsidy, people will purchase and consume larger quantities of healthy food. All but one program produced significant increases in healthy food consumption. This shows that healthy food subsidies can be an effective means of changing dietary behaviour. These programs did not conclusively link subsidies to changes in population-level BMI, however.
Policy Choice 2: Exercise
Certainly, the cost of joining a gym is a barrier – but if the government subsidized exercise facilities, as the City of Calgary does, would low-income earners participate more often? People earning lower incomes are hard pressed to substitute work for leisure activities, such as exercise. This suggests that earning a lower hourly wage necessitates working more hours to make ends meet. There is also evidence suggesting that cost is one of many factors influencing the choice to exercise. The choice to exercise is dependant on psychological and social environmental conditions. For the government, addressing the fear of physical pain, or social stigma must be included in exercise promotion programs, to eliminate both financial and psychosocial barriers.
The Big Picture
Choosing to enact policies that target individual obesity factors has not produced a substantial shift in population-level BMI distribution. Taxpayers might prefer a simple government policy, but in this case, a quick-fix approach will not work. The Canadian government has failed to communicate the complexity of the obesity problem to the electorate. It is difficult for most of us to understand how the country could benefit from a new national program: one that includes an income-based exercise program, an overhaul of the Canada Food Guide, and a new taxation-subsidy regime.
To the electorate, this means more tax dollars going towards an issue with which most don’t identify. If, by 2025, 34% of Canadians are obese, the CCHS suggests that, of that 34%, most will be low to no-income. For the most part, non-obese citizens will pay for these programs. Since obesity is associated with poor workforce productivity and increasing public healthcare system costs, the government needs to take decisive action, regardless of the policy’s popularity. Complex multivariate policies are difficult to implement, which explains the affinity for quick-fix policies. However, as I’ve demonstrated, simple policies cannot solve complex problems. Even if the government addresses either diet or exercise, this will raise a host of other issues. Without multivariate policies, the obesity problem will persist, and 34% of the population will be obese by 2025.